The most common question about root canal treatment? “Will it hurt?” Despite decades of outdated stories creating fear, modern root canal therapy is genuinely painless when performed with proper anesthesia and advanced techniques. In fact, the procedure eliminates severe tooth pain rather than causing it—relieving the infection that creates your discomfort while preserving your natural tooth.
In Abu Dhabi, where dental healthcare meets international standards of excellence, painless root canal treatment has become the standard. Advanced anesthetic techniques, rotary endodontic instruments, and specialist expertise combine to deliver comfortable care that saves teeth extraction would otherwise claim. This comprehensive guide explains exactly why modern root canal treatment is painless, what the procedure entails, and how to ensure the smoothest possible experience.
At Al Bustan Medical Group, our MOHAP-licensed endodontic specialists have performed thousands of successful, comfortable root canal treatments over 18 years. Using advanced technology and gentle techniques, we’ve helped patients discover that root canal treatment doesn’t match its fearsome reputation—it’s simply effective tooth preservation. This guide draws on that extensive clinical experience to provide the honest, detailed information you need.
Understanding Root Canal Treatment: The Basics
Root canal treatment—also called endodontic therapy—removes infected or damaged tissue from inside a tooth, then seals the internal spaces to prevent reinfection. Despite the procedure’s intimidating reputation, it actually relieves severe tooth pain rather than causing it, addressing the underlying infection that creates discomfort.
Tooth Anatomy: Why Root Canals Become Necessary
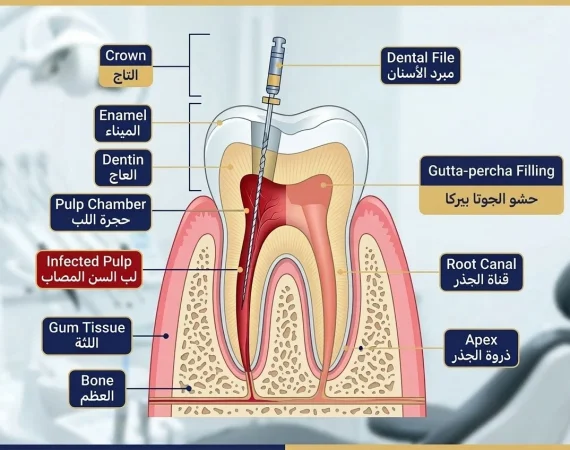
Understanding tooth structure clarifies why root canal treatment sometimes becomes essential. Each tooth contains multiple layers serving different functions.
Enamel: The hard, visible outer layer protects underlying structures. Enamel contains no living cells or nerves, which is why cavity drilling in enamel doesn’t hurt. However, once decay penetrates through enamel into deeper layers, problems begin.
Dentin: The layer beneath enamel contains microscopic tubules connecting to the nerve. Decay or damage reaching dentin causes sensitivity and discomfort as bacteria approach the pulp chamber.
Pulp: The soft tissue core of each tooth contains blood vessels, nerves, and connective tissue. During tooth development, pulp creates dentin and nourishes the growing tooth. In mature teeth, pulp serves primarily sensory functions. When bacteria reach the pulp through deep decay, cracks, or trauma, infection develops.
Root Canals: These narrow channels run from the pulp chamber through each root to the tip, where blood vessels and nerves enter the tooth. Teeth contain one to four roots depending on their position and function. Molars typically have three to four canals, while front teeth usually have one.
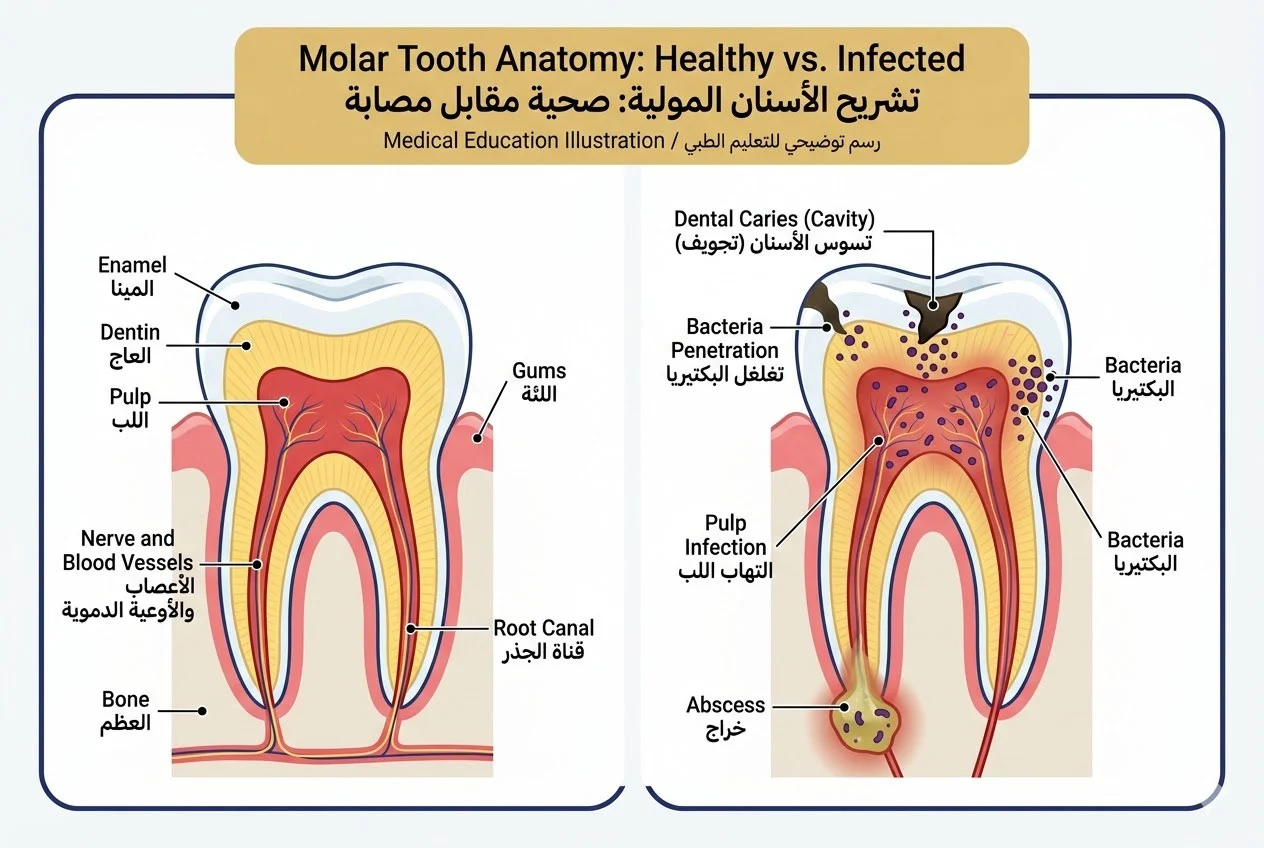
What Happens When Pulp Becomes Infected
Dental pulp infection or inflammation—called pulpitis—occurs when bacteria invade the pulp chamber. This can result from several causes: deep untreated cavities, cracks or chips exposing pulp, repeated dental procedures on the same tooth, or trauma that damages pulp even without visible cracks.
Initially, pulpitis may be reversible if caught early and treated promptly. However, once infection becomes established, the pulp cannot heal itself. The confined space inside the tooth provides ideal conditions for bacteria to multiply, creating pressure and severe pain. Without intervention, infection spreads through the root canal system into surrounding bone, potentially forming an abscess—a pocket of pus at the root tip.
Abscessed teeth create severe, throbbing pain, facial swelling, fever, and general illness. In rare cases, untreated dental infections can spread to other parts of the body, creating serious health complications. Root canal treatment halts this progression by removing the infected tissue and sealing the tooth against reinfection.
Signs You Might Need Root Canal Treatment
Recognizing symptoms that may indicate pulp infection helps you seek treatment before complications develop. While only a dental professional can definitively diagnose the need for root canal treatment, certain warning signs suggest pulp problems requiring evaluation.
Common Symptoms Requiring Evaluation
Severe Toothache: Intense, persistent pain that worsens with chewing or pressure often indicates pulp infection. The pain may be constant or intermittent, sometimes waking you at night. Pain that increases when lying down suggests advanced infection.
Prolonged Sensitivity: Lingering sensitivity to hot or cold temperatures—particularly pain that continues after the stimulus is removed—suggests pulp inflammation. Normal sensitivity resolves within seconds; pulpitis pain lingers for minutes or longer.
Swelling and Tenderness: Gum swelling near a particular tooth, especially accompanied by tenderness or a pimple-like bump on the gums, often indicates infection draining from the root tip. The swelling may come and go as infection cycles through active and dormant phases.
Tooth Discoloration: Darkening or graying of a tooth suggests pulp death, often following trauma that damaged blood vessels. While discolored teeth don’t always require root canals, the change warrants examination.
Persistent Bad Taste: An unpleasant taste or odor that localizes to a specific tooth may indicate infection draining into the mouth through a tiny opening in the gum.
Pain When Chewing: Discomfort when biting down on a specific tooth suggests infection at the root tip, where pressure aggravates inflamed tissues surrounding the tooth.
When Symptoms Don’t Match Severity
Interestingly, not all infected teeth cause dramatic symptoms. Some people experience minimal discomfort despite significant infection—a phenomenon called chronic pulpitis. These cases often surprise patients when X-rays reveal abscesses, as they’ve adapted to low-level discomfort.
Conversely, some patients experience severe symptoms from inflammation that hasn’t progressed to full infection. Early intervention in these cases may occasionally save pulp vitality through less invasive treatments. This underscores the importance of professional evaluation rather than self-diagnosis based on pain alone.
The Root Canal Procedure: Step-by-Step
Understanding what happens during root canal treatment demystifies the procedure and reduces anxiety. Modern techniques have transformed root canal treatment into a comfortable, predictable process quite different from outdated methods that earned the procedure its negative reputation.
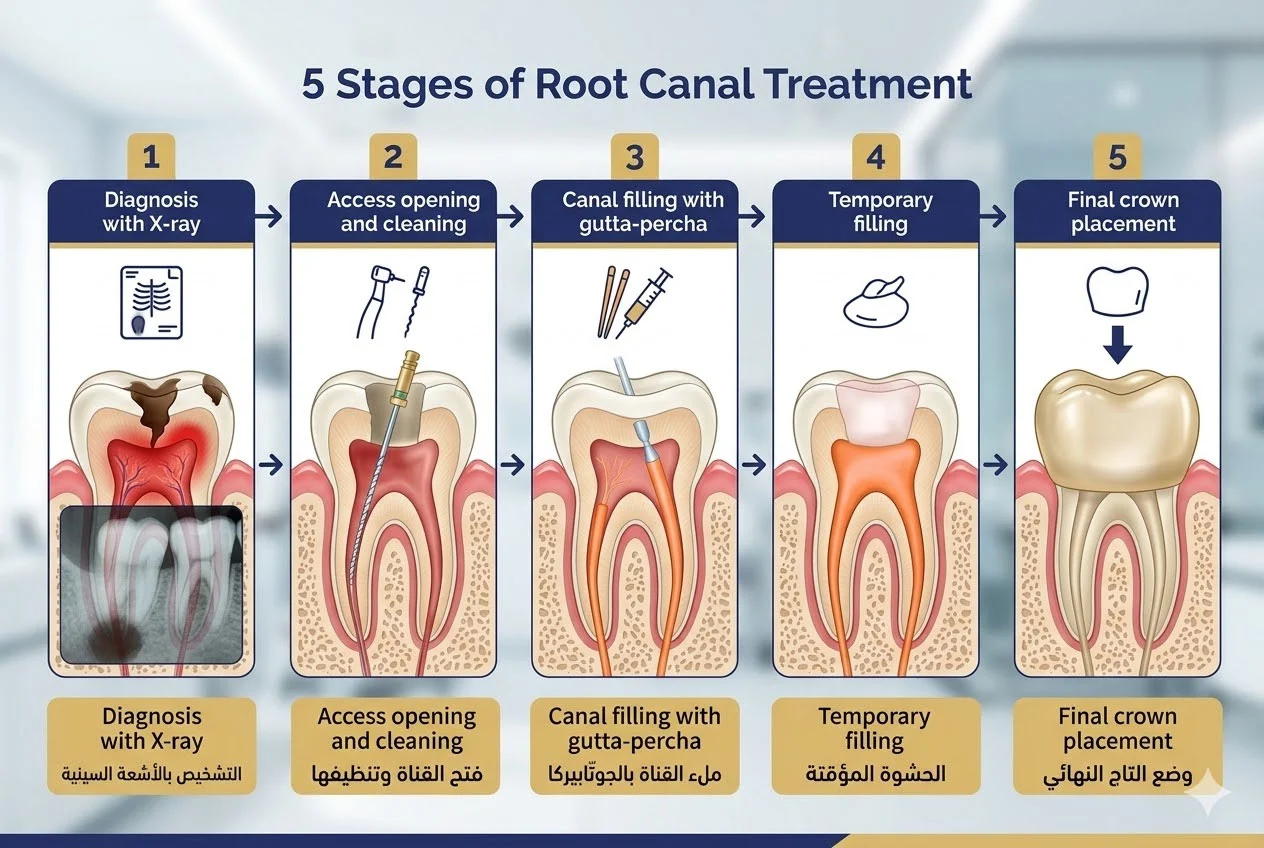
Diagnosis and Treatment Planning
Root canal treatment begins with thorough examination and imaging. Your endodontist examines the affected tooth, reviews your symptoms, and takes diagnostic X-rays or 3D scans to visualize root canal anatomy and assess infection extent. This information guides treatment planning.
The number of canals, their configuration, and the presence of calcification or unusual anatomy all influence treatment complexity. Some teeth present straightforward anatomy, while others require advanced techniques and additional time. Digital imaging helps endodontists anticipate challenges and plan accordingly.
Appointment One: Accessing and Cleaning the Canals
Anesthesia: Contrary to popular belief, root canal treatment itself causes no pain. Local anesthetic thoroughly numbs the tooth and surrounding tissues before any work begins. You may feel pressure during the procedure but should experience no pain. If you do feel discomfort, additional anesthetic can be administered immediately.
Isolation: A rubber dam—a thin sheet of latex or non-latex material—isolates the tooth being treated. This keeps saliva and bacteria away from the work area while providing a comfortable barrier between your mouth and dental instruments. While the dam feels unusual, it improves comfort by preventing instruments or irrigation solutions from touching your tongue or cheeks.
Access Opening: The endodontist creates a small opening in the tooth’s chewing surface (or the back of a front tooth) to access the pulp chamber. This opening allows instruments to reach the canals for cleaning.
Canal Cleaning: Using specialized instruments called endodontic files, the endodontist removes infected pulp tissue, bacteria, and debris from the canals. Modern rotary files—tiny flexible instruments powered by a precision motor—clean canals more efficiently and comfortably than hand files used in the past.
The cleaning process involves gradually increasing file sizes to shape canals while removing all diseased tissue. Throughout cleaning, the endodontist irrigates canals with antibacterial solutions that flush debris and disinfect the canal system. This chemical cleaning complements mechanical cleaning for thorough disinfection.
Measuring Canal Length: Precise measurements ensure cleaning reaches the canal’s entire length without extending beyond the root tip into surrounding bone. Electronic apex locators provide accurate measurements, supplemented by X-rays for verification.
Temporary Filling: Once canals are thoroughly cleaned and dried, the endodontist places medication inside to eliminate any remaining bacteria. A temporary filling seals the access opening, protecting the tooth between appointments. In some cases, particularly when infection is extensive, this medication remains in place for a week or two before permanent filling.
Appointment Two: Permanent Canal Filling
The second appointment typically occurs one to two weeks after initial treatment, allowing medication time to work. However, in many cases, root canals can be completed in a single visit if infection is minimal and anatomy is straightforward.
Final Cleaning: The endodontist removes temporary filling and medication, then performs final irrigation and cleaning to ensure complete disinfection.
Canal Filling: Root canals are filled with a rubber-like material called gutta-percha, which seals the canals against future bacterial invasion. Gutta-percha is heated slightly and compressed into the canals, creating a dense, three-dimensional seal from the canal orifice to the root tip. A sealer cement accompanies the gutta-percha, filling any microscopic gaps.
Access Sealing: The access opening is sealed with a permanent filling material. However, this filling is temporary in nature—the tooth requires a crown for long-term protection and function.
Verification X-ray: A final X-ray confirms that canals are filled completely to the proper length, with no voids or gaps that could allow reinfection.
Follow-Up: Crown Placement
Root canal treatment removes not only pulp but also significant tooth structure during access and preparation. This weakens the tooth, making it susceptible to fracture under normal chewing forces. A dental crown—a custom-fitted cap covering the entire tooth—protects the tooth and restores full function.
Crown placement typically occurs two to four weeks after root canal completion, allowing time to ensure the tooth settles comfortably. Your general dentist or prosthodontist prepares the tooth for a crown, takes impressions, and places a temporary crown while your permanent crown is fabricated. At a subsequent appointment, the permanent crown is cemented in place, completing restoration.
Does Root Canal Treatment Hurt?
The answer is simple: No. When performed with proper anesthesia and modern techniques, root canal treatment is painless. The procedure’s fearsome reputation comes from outdated methods and untreated infections—not from the treatment itself. In fact, root canal therapy eliminates the severe pain caused by infection rather than creating pain.
Understanding what makes modern root canal treatment genuinely painless helps separate fact from decades-old fiction.
During Treatment: It Doesn’t Hurt
Properly administered local anesthetic completely numbs the tooth and surrounding tissues before any work begins. Root canal treatment performed under adequate anesthesia causes zero pain—only pressure and vibration sensations as instruments work inside the tooth. If you feel any pain during treatment, it indicates insufficient anesthesia, which your endodontist can immediately address with additional anesthetic.
Some teeth prove challenging to anesthetize completely, particularly severely infected lower molars. This occurs because inflammation affects how anesthetic works, and lower jaw anatomy sometimes requires supplemental injection techniques. Experienced endodontists anticipate these challenges and use additional anesthetic methods to ensure comfort.
After Treatment: Normal Post-Procedure Discomfort
Some tenderness after root canal treatment is normal and expected. You’re likely to experience:
Mild to Moderate Soreness: The tooth and surrounding gum may feel tender when you bite down or touch the area. This results from manipulation of tissues around the root tip during cleaning and filling. The soreness typically peaks within 24-48 hours after treatment, then gradually subsides over three to seven days.
Jaw Fatigue: Keeping your mouth open during treatment can make jaw muscles sore, similar to fatigue after a long dental appointment. This usually resolves within a day or two.
Gum Sensitivity: The rubber dam clamp and instruments may create minor gum irritation that heals quickly.
Over-the-counter pain relievers like ibuprofen effectively manage this normal post-treatment discomfort. Most patients return to normal activities immediately, taking medication as needed for a few days.
When Post-Treatment Pain Indicates Problems
While mild discomfort is expected, certain symptoms warrant contacting your endodontist:
• Severe pain that worsens rather than improving over the first few days
• Swelling that increases or spreads to your face or neck
• Fever or general illness
• Visible swelling inside or outside your mouth
• An allergic reaction to prescribed medication
• Temporary filling or crown coming loose or falling out
• Bite feeling significantly uneven after anesthetic wears off
These symptoms are uncommon but require prompt evaluation to address any complications early. Most resolve with simple interventions when caught quickly.
Recovery and Aftercare: What to Expect
Proper aftercare ensures optimal healing and long-term success of root canal treatment. Following these guidelines minimizes discomfort and complications.
Immediate Post-Treatment Care (First 24-48 Hours)
Wait for Anesthetic to Wear Off: Avoid eating until numbness completely resolves to prevent accidentally biting your cheek, tongue, or lips. This typically takes two to four hours after treatment.
Manage Discomfort: Take pain medication before anesthetic wears off completely. Staying ahead of discomfort prevents pain from becoming severe. Use medications as prescribed or recommended—typically ibuprofen or a combination of ibuprofen and acetaminophen for more significant discomfort.
Eat Soft Foods: Choose soft, easy-to-chew foods for the first day or two. Avoid hard, crunchy, or sticky foods that could stress the treated tooth or dislodge temporary filling.
Chew on the Opposite Side: Use the untreated side of your mouth for chewing until permanent restoration is placed. This protects the treated tooth from excessive force.
Apply Cold Compresses: If facial swelling occurs, apply ice packs to the outside of your face for 15-minute intervals during the first 24 hours. This reduces inflammation and provides comfort.
Ongoing Care Until Crown Placement
Protect the Tooth: Avoid chewing hard foods or ice with the treated tooth. Without a crown, the tooth remains vulnerable to fracture despite successful root canal treatment.
Maintain Oral Hygiene: Brush and floss normally, including around the treated tooth. Good oral hygiene supports healing and prevents complications.
Monitor the Temporary Filling: Temporary fillings aren’t designed for long-term wear. If it feels loose or falls out before your crown appointment, contact your dentist promptly. Don’t delay crown placement—prolonged waiting increases fracture risk and may allow reinfection.
Attend Follow-Up Appointments: Don’t skip your crown appointment. Even if the tooth feels fine, it requires permanent restoration for long-term success.
Long-Term Care After Crown Placement
Once crowned, root canal-treated teeth function like natural teeth and can last a lifetime with proper care:
• Maintain excellent oral hygiene with twice-daily brushing and daily flossing
• Attend regular dental checkups and cleanings every six months
• Avoid using teeth as tools to open packages or crack nuts
• Wear a nightguard if you grind your teeth during sleep
• Address any new dental problems promptly to prevent complications
Root canal-treated teeth remain subject to new cavities, gum disease, and fractures like any other tooth. Ongoing preventive care protects your investment in treatment.
Success Rates and Long-Term Outcomes
Root canal treatment boasts impressive success rates when performed properly and followed by appropriate restoration. Understanding factors affecting outcomes helps patients maximize treatment success.
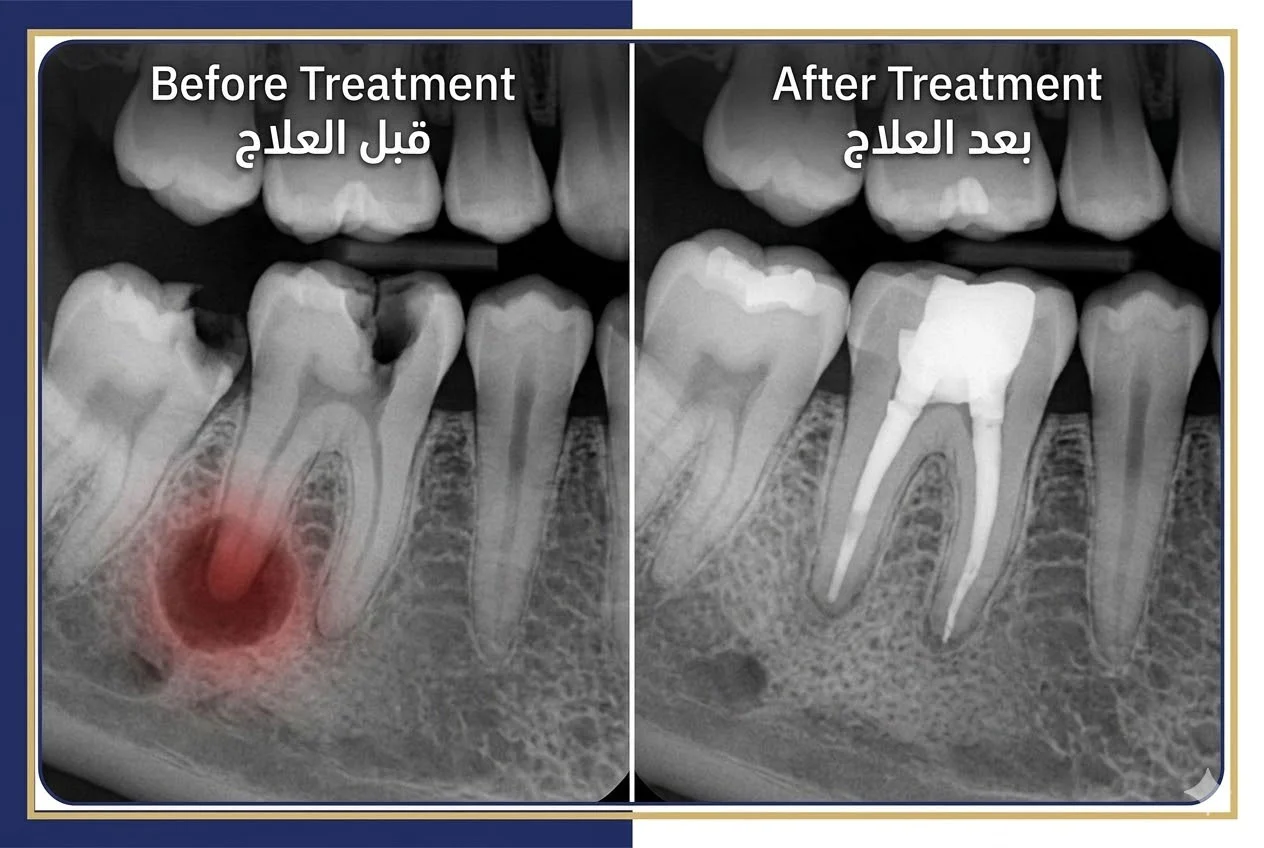
What “Success” Means
Successful root canal treatment means the tooth remains functional, comfortable, and free of infection indefinitely. X-rays show healthy bone around root tips, with no signs of abscess or reinfection. The tooth withstands normal chewing forces without pain or mobility.
Studies consistently show 85-97% success rates for initial root canal treatment, with success defined as absence of symptoms and radiographic healing after several years. These high rates reflect modern techniques, materials, and equipment that have dramatically improved treatment precision and outcomes.
Factors Affecting Success
Treatment Quality: Thorough cleaning, complete filling, and proper sealing are critical. Missed canals or inadequate cleaning leave bacteria that can cause reinfection. Complex anatomy requires specialized expertise to achieve complete disinfection.
Crown Placement: Teeth that don’t receive crowns after root canal treatment have significantly higher failure rates due to fracture. The crown protects remaining tooth structure and seals the access opening against bacterial penetration.
Tooth Location and Condition: Front teeth generally have higher success rates than molars due to simpler anatomy with fewer canals. Teeth with extensive infection or previous root canal treatment have slightly lower success rates than first-time treatments on teeth with minimal infection.
Patient Factors: Overall health, immune function, and oral hygiene habits all influence outcomes. Conditions like diabetes can slightly reduce success rates, though treatment still succeeds in the majority of cases with good disease management.
When Retreatment Becomes Necessary
Sometimes root canal-treated teeth develop problems months or years later, requiring retreatment. This can occur because of new decay exposing canals to bacteria, delayed crown placement allowing reinfection, or missed canals during initial treatment.
Endodontic retreatment involves removing the previous filling material, cleaning and disinfecting canals again, and refilling them. Success rates for retreatment remain good—typically 70-90%—though slightly lower than initial treatment. The alternative is extraction, so retreatment is generally worth attempting when problems develop.
Alternatives to Root Canal Treatment
When infection threatens a tooth, root canal treatment isn’t the only option, though it’s usually the preferred one. Understanding alternatives helps patients make informed decisions about tooth preservation versus extraction.
Tooth Extraction
Removing the infected tooth eliminates the problem but creates other consequences. Missing teeth cause adjacent teeth to shift, alter bite relationships, reduce chewing efficiency, and may affect facial appearance if front teeth are involved. Bone loss occurs in the extraction site over time, potentially complicating future tooth replacement.
Replacing extracted teeth requires dental implants, bridges, or partial dentures—all more expensive and invasive than root canal treatment plus crown. While extraction may seem like a simpler, cheaper option initially, long-term costs and consequences typically exceed those of saving the natural tooth.
Extraction makes sense in certain situations: teeth with vertical root fractures that can’t be restored, teeth with insufficient bone support due to advanced gum disease, or teeth whose root canal anatomy makes successful treatment impossible.
Pulpotomy
This partial pulp removal removes only the coronal (crown) portion of pulp while leaving root pulp intact. Pulpotomy works primarily in children’s primary teeth or young permanent teeth with immature roots. It’s inappropriate for mature adult teeth with pulp infection, which require complete pulp removal.
Watchful Waiting
Delaying treatment while monitoring symptoms is generally inadvisable once infection is diagnosed. Infections don’t resolve spontaneously—they worsen, potentially spreading to surrounding structures or becoming more difficult to treat. What starts as inflammation requiring routine root canal treatment can progress to severe infection requiring emergency intervention, antibiotics, or even hospitalization in extreme cases.
The only scenario where monitoring makes sense is reversible pulpitis caught extremely early, where removing decay and placing a restoration might allow pulp to heal. Your dentist can assess whether this conservative approach is viable or whether definitive treatment is necessary.
Root Canal Treatment at Al Bustan Medical Group
For 18 years, Al Bustan Medical Group has provided comprehensive endodontic care to Abu Dhabi families, combining advanced technology with specialized expertise to deliver comfortable, successful root canal treatment.
Our Endodontic Specialists
Two dedicated endodontic specialists provide root canal treatment across our network:
At Al Bustan Medical Center (Khalifa City): Dr. Wafaa Youniss, Specialist Endodontist, brings extensive experience in complex root canal cases, retreatment, and traumatic dental injuries requiring endodontic intervention.
At Al Bustan Advance Medical Center (Khalifa City): Dr. Rasha Helamieh, Specialist Endodontist, specializes in difficult cases involving calcified canals, unusual anatomy, and teeth requiring microsurgical endodontics.
Both specialists maintain MOHAP licensing and participate in continuing education to stay current with evolving endodontic techniques and technologies.
Advanced Technology for Precision and Comfort
Rotary Endodontics: Computer-controlled rotary instruments clean and shape canals more efficiently than traditional hand files, reducing procedure time while improving cleaning thoroughness. The gentle, continuous motion creates less vibration and discomfort than older techniques.
Electronic Apex Locators: These devices precisely measure canal length electronically, reducing the number of X-rays needed during treatment while ensuring accurate working lengths.
Digital Radiography: Instant digital X-rays use up to 90% less radiation than traditional film X-rays while providing superior image quality for diagnosis and treatment verification.
Dental Microscopes: High-powered magnification and illumination allow endodontists to visualize tiny canal openings and anatomical details invisible to the naked eye, improving treatment precision especially in complex cases.
Comprehensive Approach to Patient Comfort
We recognize that anxiety about root canal treatment stems from outdated perceptions and fear of the unknown. Our approach prioritizes comfort through:
• Thorough explanation of each step before proceeding, ensuring you understand what to expect
• Gentle anesthetic techniques that minimize injection discomfort
• Additional anesthetic options if you feel any discomfort during treatment
• Breaks during longer procedures to rest your jaw and reposition comfortably
• Post-treatment instructions and medications to manage normal healing discomfort
• Clear communication about when and how to contact us if concerns arise
Convenient Locations and Extended Hours
Root canal treatment is available at multiple Al Bustan Medical Group locations across Abu Dhabi. Our extended hours—9:00 AM to 10:00 PM daily—accommodate work schedules and urgent dental needs. Emergency dental appointments are available for severe tooth pain or dental trauma requiring immediate attention.
Whether you need routine endodontic treatment or complex retreatment, our specialists provide consistent, high-quality care regardless of which location you visit. Call 8007755 or book online to schedule your evaluation.
Cost Considerations
Root canal treatment costs vary based on several factors, with transparent pricing helping patients plan for necessary care.
Factors Affecting Treatment Cost
Tooth Location: Front teeth (incisors and canines) typically have one or two canals and simpler anatomy, making treatment more straightforward. Premolars have one or two canals with moderate complexity. Molars have three to four canals with complex, curved anatomy requiring more time and expertise. Consequently, molar root canals cost more than front tooth treatment.
Treatment Complexity: Unusual anatomy, calcified canals, or previous root canal treatment requiring removal and replacement of existing filling all increase treatment complexity and cost. Teeth with severe infection or abscesses may require additional appointments and medication, affecting overall investment.
Specialist vs. General Dentist: While general dentists can perform many root canal treatments, complex cases benefit from endodontist expertise. Specialist fees reflect advanced training, specialized equipment, and the ability to handle difficult cases that might otherwise fail.
Crown Requirements: The crown needed after root canal treatment represents a separate cost from the endodontic procedure itself. Crown type (porcelain-fused-to-metal, all-ceramic, or gold) affects this portion of total treatment expense.
Comparing Root Canal Cost to Alternatives
While root canal treatment plus crown represents a significant investment, it typically costs less than tooth replacement options while preserving your natural tooth:
• Extraction plus dental implant usually exceeds root canal treatment cost substantially
• Bridges require preparing adjacent teeth, increasing complexity and expense
• Partial dentures are less expensive initially but require periodic replacement and adjustments
• Nothing functions as well as your natural tooth when properly restored
When evaluating cost, consider long-term value rather than just immediate expense. A successfully treated tooth can last a lifetime, while extractions create ongoing complications and costs.
Insurance and Payment Options
Dental insurance coverage for root canal treatment varies by plan. Many plans classify endodontic treatment as a major procedure, covering 50-80% of costs after deductibles. Crown coverage follows similar patterns. Our administrative staff verifies coverage before treatment, providing detailed cost estimates based on your specific benefits.
For patients without insurance or those seeking to spread costs over time, we offer flexible payment arrangements that make necessary treatment accessible. Investing in tooth preservation now prevents more expensive complications later.
Preventing the Need for Root Canals
While root canal treatment successfully saves infected teeth, prevention remains the ideal approach. Understanding what causes pulp infections helps you protect your teeth proactively.
Primary Prevention Strategies
Treat Cavities Promptly: Deep decay is the most common cause of pulp infection. Address cavities when they’re small and confined to enamel or superficial dentin. Small fillings prevent decay from reaching pulp, eliminating the most frequent reason for root canal treatment.
Maintain Excellent Oral Hygiene: Brush twice daily with fluoride toothpaste and floss daily to prevent cavity formation. Regular cleaning removes bacterial plaque before it produces acids that create decay.
Attend Regular Dental Checkups: Professional examinations every six months catch problems early. Dentists identify cavities in early stages when simple fillings suffice, preventing progression to pulp involvement.
Use Protective Sports Guards: Athletic activities create risk of dental trauma. Custom mouthguards protect teeth from fractures and impacts that can damage pulp even without visible cracks.
Address Teeth Grinding: Chronic grinding or clenching creates microfractures in enamel that can propagate to deeper structures over time. Nightguards protect teeth from excessive forces that contribute to cracks and eventual pulp exposure.
Avoid Using Teeth as Tools: Opening packages, cracking nuts, or holding objects with teeth creates unnecessary stress that can cause fractures. Use appropriate tools instead of risking tooth damage.
When Prevention Isn’t Enough
Despite best preventive efforts, some situations increase root canal risk regardless of oral care quality:
• Genetic factors affecting enamel strength or cavity susceptibility
• Accidents causing dental trauma
• Previous large fillings that eventually fail, allowing decay to reach pulp
• Medical conditions or medications that reduce saliva flow, increasing cavity risk
If root canal treatment becomes necessary despite preventive efforts, view it as a valuable procedure that saves your tooth rather than a failure of oral care. The goal is preserving natural teeth, and endodontic treatment achieves that when needed.

Frequently Asked Questions: Root Canal Treatment
Q: How long does root canal treatment take?
Most root canal treatments require one or two appointments, each lasting 60-90 minutes depending on tooth complexity. Front teeth with single canals often complete in one visit, while molars with multiple complex canals may require two appointments. Between appointments (if two are needed), medication remains in the tooth for one to two weeks. Crown placement occurs two to four weeks after root canal completion at a separate appointment with your general dentist.
Q: Can I drive myself home after root canal treatment?
Yes, you can drive after root canal treatment since only local anesthetic is used. The procedure doesn’t impair your ability to drive safely. However, plan to take it easy for the rest of the day, as some people feel tired after dental appointments due to stress relief following treatment.
Q: Will my tooth be weaker after root canal treatment?
The tooth becomes slightly more brittle after root canal treatment because the procedure removes internal structures including blood supply. However, a properly placed crown protects the tooth and distributes chewing forces evenly, allowing it to function like a natural tooth indefinitely. Without a crown, root canal-treated teeth are indeed vulnerable to fracture—which is why crown placement is essential for long-term success.
Q: Do I need antibiotics before or after root canal treatment?
Most patients don’t require antibiotics for routine root canal treatment. The procedure removes infection directly by eliminating bacteria from the canal system. However, antibiotics may be prescribed if you have severe swelling, fever, systemic symptoms, or certain medical conditions requiring antibiotic prophylaxis for dental procedures. Your endodontist will determine whether antibiotics are appropriate for your situation.
Q: Can root canal treatment be done in one visit?
Yes, many root canals can be completed in a single appointment, particularly when treating front teeth with straightforward anatomy or teeth without severe infection. One-visit root canal treatment uses the same techniques as two-visit treatment—the difference is that cleaning, disinfection, and filling occur in one session rather than being separated by a medication period. Your endodontist determines whether single-visit treatment is appropriate based on infection severity and canal complexity.
Q: What happens if I delay getting a root canal when it’s recommended?
Delaying necessary root canal treatment allows infection to worsen and spread. You may experience increasing pain, facial swelling, fever, and difficulty eating or sleeping. The infection can create an abscess that drains into the mouth or spreads to surrounding tissues. In severe cases, dental infections can become life-threatening if bacteria enter the bloodstream. Additionally, delayed treatment may make the root canal more complex or reduce success rates. In extreme cases, delay may progress beyond the point where root canal treatment can save the tooth, necessitating extraction instead.
Q: Can children have root canal treatment?
Yes, though the procedure differs slightly for children’s primary (baby) teeth versus permanent teeth. For baby teeth, a pulpotomy—which removes only the crown portion of pulp—often suffices since these teeth will eventually fall out naturally. For children’s permanent teeth, full root canal treatment preserves teeth that need to last a lifetime. Pediatric dentists or endodontists experienced with children ensure comfortable treatment appropriate to the child’s age and dental development.
Q: How do I know if I need root canal treatment or just a filling?
Only a dentist can definitively determine whether decay requires a simple filling or root canal treatment. Generally, cavities confined to enamel and outer dentin layers require only fillings. When decay reaches pulp or causes pulp inflammation, root canal treatment becomes necessary. Diagnostic tests—including response to temperature, percussion tests, and X-rays showing infection at root tips—guide this determination. If symptoms include severe pain, prolonged sensitivity, or spontaneous throbbing, root canal treatment is more likely needed than a simple filling.
Q: Can a root canal-treated tooth get infected again?
While uncommon, reinfection can occur if new decay allows bacteria to reenter the canal system, if the permanent crown is delayed allowing saliva contamination, or if canals weren’t completely sealed during initial treatment. Reinfection symptoms mirror original infection—pain, swelling, and sensitivity. Retreatment involves removing existing filling material, re-cleaning canals, and refilling them. Success rates for retreatment remain good (70-90%), though slightly lower than initial treatment. Proper crown placement and ongoing oral care minimize reinfection risk.
Q: Is it normal for my tooth to hurt after root canal treatment?
Mild to moderate soreness for several days after root canal treatment is completely normal. This discomfort results from inflammation at the root tip where instruments cleaned the canal and from manipulation of surrounding tissues. Pain typically peaks within 24-48 hours then gradually improves over three to seven days. Over-the-counter pain relievers usually provide adequate relief. However, severe pain that worsens rather than improving, significant swelling, or fever are not normal and require prompt evaluation to rule out complications.
Q: Why do I need a crown after root canal treatment?
Root canal treatment removes substantial tooth structure—not only the pulp but also enamel and dentin removed to access canals. This leaves the tooth walls thin and brittle, vulnerable to fracture under normal chewing forces. A crown caps the entire tooth, distributing forces evenly and protecting remaining structure from breaking. Studies show root canal-treated teeth without crowns have significantly higher failure rates due to fracture. While the tooth may feel fine without a crown initially, fracture risk remains high and increases over time. Crown placement is essential for long-term success, not optional.
Q: How successful is root canal treatment at Al Bustan Medical Group?
Our endodontic specialists achieve success rates consistent with international standards—85-97% for initial root canal treatment. Success depends on factors including tooth condition, infection severity, canal complexity, and patient factors like overall health and oral hygiene. Our use of advanced technology including rotary endodontics, electronic apex locators, and dental microscopes optimizes outcomes. When combined with proper crown placement and ongoing oral care, root canal-treated teeth can last a lifetime. Regular follow-up examinations monitor healing and catch any problems early.
Taking the Next Step
Root canal treatment represents modern dentistry’s best option for saving teeth threatened by infection. While the procedure carries an outdated reputation for discomfort, contemporary techniques have transformed it into a comfortable, predictable process that relieves pain rather than causing it.
If you’re experiencing tooth pain, sensitivity, or other symptoms suggesting pulp problems, prompt evaluation prevents complications and often makes treatment simpler. Delaying necessary care allows infections to worsen and may ultimately compromise your ability to save the tooth.
At Al Bustan Medical Group, our MOHAP-licensed endodontic specialists provide expert root canal treatment using advanced technology and gentle techniques. With 18 years of experience and nine convenient Abu Dhabi locations, we make quality endodontic care accessible when you need it.
Don’t let fear or misconceptions prevent you from saving your natural tooth. Schedule a consultation to discuss your symptoms and explore your options. Call 8007755 or book online for an appointment that fits your schedule.
Al Bustan Medical Group: 18 years of trusted endodontic care, nine convenient Abu Dhabi locations, MOHAP-licensed specialists, advanced technology. Your natural tooth is worth saving.